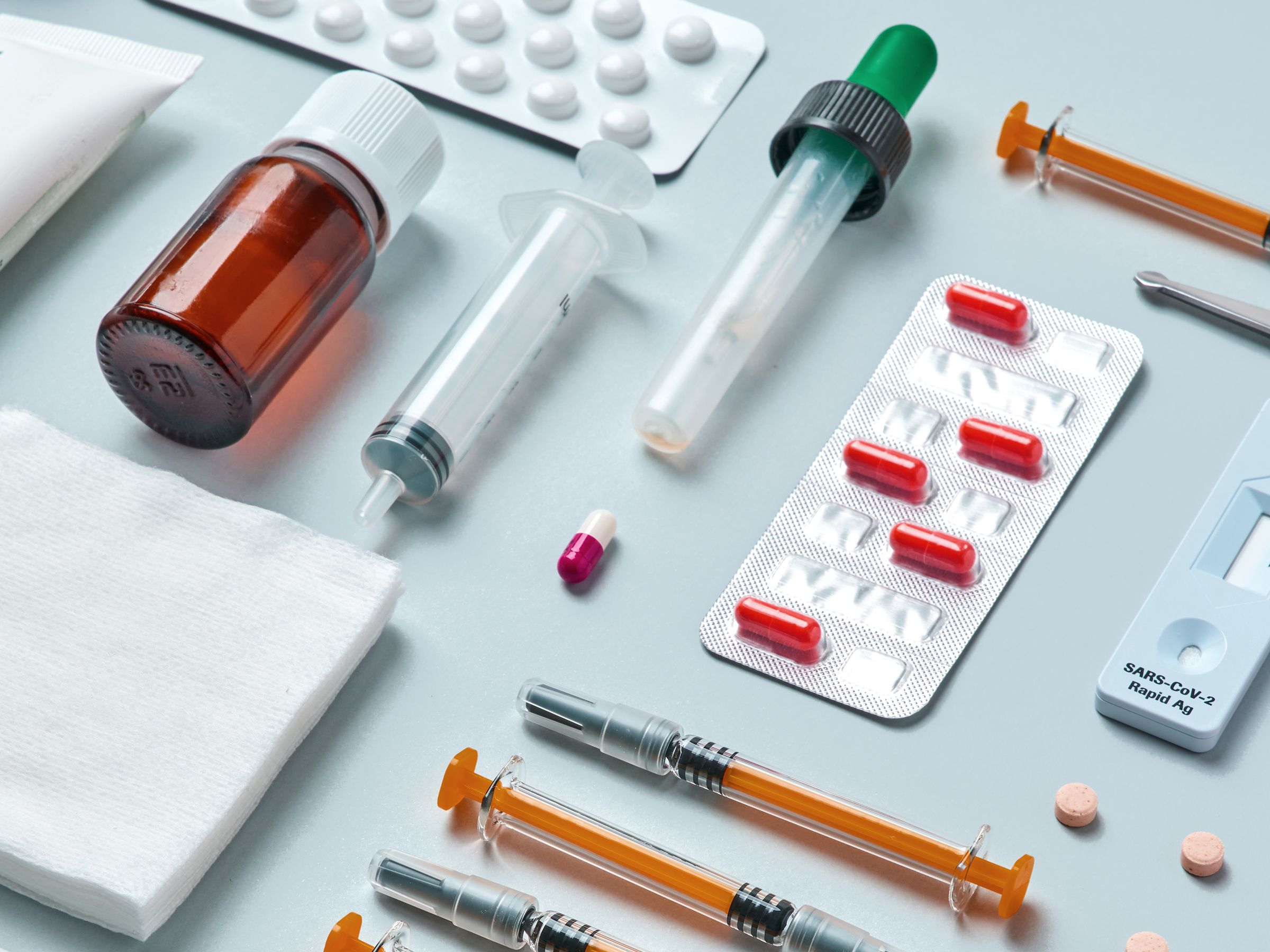
The Urgency of Enhanced Diabetes Detection
Diabetes affects millions worldwide, yet conventional detection methods often miss early stages, allowing irreversible damage to develop. The reliance on static blood glucose readings overlooks nuanced physiological patterns and population-specific variations that can mask risk. As global prevalence climbs, innovative solutions must address these gaps to prevent complications before they manifest.
- Current Limitations
- Blood sugar tests fail to capture long-term metabolic trends
- HbA1c yields inconsistent results across ethnic groups
- Delayed diagnosis increases complication likelihood
Emerging Technologies Redefine Screening
Researchers are integrating advanced sensors and artificial intelligence to spot early warning signs beyond conventional metrics. These developments promise earlier, more accurate identification of individuals at risk, enabling timely intervention and personalized care pathways.
-
Continuous Glucose Monitoring (CGM)
- Real-time tracking reveals hidden fluctuations invisible to occasional lab draws
- AI algorithms decode complex patterns linked to prediabetes and Type 2 onset
- Cost reductions make wearable devices increasingly accessible for routine use
-
AI-Powered ECG Analysis
- Electrocardiograms offer scalable, non-invasive screening across diverse populations
- Machine learning models achieve up to 70% accuracy in predicting future diabetes risk
- Potential integration into standard care workflows streamlines early detection
Beyond Blood Sugar: Multimodal Risk Assessment
Beyond glucose-centric approaches, new tools explore physiological signals such as heart rhythm variations to forecast disease trajectory. This holistic perspective recognizes that metabolic health intertwines with cardiovascular function, offering broader preventive opportunities.
-
Cardiovascular Insights
- Subtle ECG alterations precede measurable hyperglycemia
- Large-scale datasets train robust prediction models applicable across ethnicities
- Early alerts empower lifestyle modifications and targeted medical oversight
-
Immunological Strategies for Type 1 Prevention
- Novel immunotherapy delays autoimmune attack when detected early
- Risk calculators combine family history, genetics, autoantibody status, and clinical factors
- Expanded access to screening tools supports proactive disease management
Toward Proactive Health Management
The convergence of wearables, AI, and multimodal diagnostics marks a shift from reactive treatment to preventative healthcare. While no single solution replaces gold-standard glucose testing, layered approaches strengthen early recognition across varied demographics. As these technologies mature, widespread adoption could dramatically lower diabetes-related morbidity by catching pathology at its most treatable phase.
Health systems must prioritize integration of emerging tools into primary care workflows, ensuring equitable access and evidence-based implementation. The future of diabetes prevention lies in precision, scalability, and continuous monitoring—transforming how we identify, manage, and ultimately curb one of modern medicine’s greatest challenges.